
Is Secondhand Smoke Still a Major Risk for Lung Cancer?
Genetic Mutations and Lung Cancer in Never Smokers
Chronic Lymphocytic Leukemia (CLL)- What Patients Should Know
Are Artificial Sweeteners Linked to Cancer?
Fact vs Fiction: What Really Causes Cancer?
Obesity and Cancer: How Weight Impacts Your Risk
Does Intermittent Fasting Help in Cancer Prevention or Treatment?
Sugary Drinks and Cancer: Hidden Dangers You Should Know
Does Green Tea Help Prevent Cancer?
Processed Foods and Cancer: How Big Is the Risk?
Anti-Cancer Diet: What to Eat During Chemotherapy
Can Immunotherapy Cure Stage 4 Cancer?
Abnormal Bleeding and Uterine Cancer: What You Should Know
Warning Signs of Uterine Cancer Women Often Ignore
Does Sunscreen Prevent Skin Cancer or Increase Risk?
Breast Self-Check vs Mammogram: What Is the Difference?
Step-by-Step Guide to Breast Self-Examination at Home
Normal vs High ESR Levels: When Should You Worry?
Rectal Cancer Symptoms: Warning Signs You Shouldn't Ignore
Difference Between Colon Cancer and Colorectal Cancer
CAR-T Cell Therapy: Breakthrough in Blood Cancer Treatment
Targeted Therapy in Hemato-Oncology: A New Hope
Genetic Testing in Hemato-Oncology: Why It Matters
Difference Between Solid Tumors and Blood Cancers
Types of Blood Cancer: Leukemia, Lymphoma, and Myeloma Explained
Needle Biopsy vs Surgical Biopsy: Key Differences
How Imaging Helps in Cancer Treatment Planning
MRI vs CT Scan vs PET Scan: Which Is Better for Cancer?
How Many Doses of HPV Vaccine Do You Need?
When Do Doctors Recommend a PET CT Scan?
Can HPV Vaccine Prevent Cervical Cancer?
Hormonal Imbalances and Cancer Risk in Men
Chronic Myeloid Leukemia (CML)- Causes and Blood Test Diagnosis
Does Sugar Really Cause Cancer- Myth vs Reality
Does Microwave Food Increase Cancer Risk
Acute Myeloid Leukemia (AML)- Early Signs and Risk Factors
Acute Lymphoblastic Leukemia (ALL)- Symptoms and Diagnosis
Lifestyle Habits That Increase Cancer Risk in Men
Oral Cancer in Men- Link Between Tobacco and Cancer Risk
Can Detox Diets Prevent Cancer
Does Hair Dye Increase Cancer Risk
Do Artificial Sweeteners Cause Cancer
Ovarian Cancer Types- Epithelial vs Germ Cell Tumors
Types of Breast Cancer Explained- From DCIS to Metastatic Breast Cancer
Ewing Sarcoma- Bone Cancer Common in Children and Teens
Carcinoid Tumors of the Digestive Tract- What You Need to Know
Bile Duct Cancer (Cholangiocarcinoma)- Early Signs and Risk Factors
Is a Full-Body Scan Effective at Detecting Cancer
Why Many Cancers Are Diagnosed Late in India
Why Are Cancer Rates Increasing in Young Adults?
Liquid Biopsy: A Game-Changer in Early Cancer Detection
Personalized Cancer Vaccines: Are They the Future of Oncology?
Blood-Based Cancer Screening Tests: How Reliable Are They?
Neuroendocrine Tumors (NETs): Symptoms & Treatment
Cancer in Men Under 40: Signs That Shouldn’t Be Ignored
What Is Minimal Residual Disease (MRD)?
Can Cancer Be Detected Years Before Symptoms Appear?
How to manage Long-Term Side Effects After Cancer Treatment
Targeted Therapy vs Immunotherapy: Key Differences Explained
Microplastics, Food Packaging, and Cancer Risk
Are Sugar and Cancer Linked? Separating Facts from Myths
Can AI Identify High-Risk Cancer Patients Early?
Alcohol Consumption and Cancer: How Much Is Too Much?
Germ Cell Tumors: Types, Symptoms & Modern Treatments
Cancer in Young Adults- A Growing Concern
How Biopsy Tests Confirm Cancer Diagnosis
Imaging vs Blood Tests- Which Detect Cancer Better
How Sleep Patterns Affect Cancer Risk
Digestive Issues That May Signal Gastrointestinal Cancers
Unexplained Weight Loss Could It Be Cancer
Can Preventive Health Checkups Detect Cancer Early
How Often Should You Get Cancer Screening Tests
Cancer Screening for People with No Symptoms
Genetic Testing for Cancer- Who Should Consider It
How Routine Blood Tests Can Indicate Hidden Cancers
What Is Surgical Oncology: Understanding the Types of Cancer Surgeries
Understanding Chemotherapy Treatment: Process, Benefits & Risks
Understanding the Types of Radiation Therapy Used in Cancer Treatment
Understanding Medical Oncology and the Role of a Medical Oncologist
IMRT, IGRT & SRS: Advanced Radiation Techniques Explained
Bone Marrow Transplant: Types, Procedure & Success Rate
How AI & Robotics Are Transforming Cancer Surgeries
Can Diet & Lifestyle Influence Blood Cancer Risk?
Why Prostate Cancer Often Goes Unnoticed: Early Signs Men Ignore
What Causes Colorectal Cancer? Understanding Major Risk Factors
How Early Menarche & Late Menopause Influence Uterine Cancer Risk
Colon vs. Rectal Cancer: What’s the Difference?
Bladder Cancer in Women – Signs, Symptoms and Treatments
Why Younger Women Are Seeing Rising Breast Cancer Rates
Early Cancer Symptoms That Require an Immediate Oncology Consultation
Can Air Pollution Cause Lung Cancer in Non-Smokers?
How to Detect Cancer Early: Screening Tests Every Adult Should Know About
Cost of Cancer Treatment in India: Chemotherapy, Radiation & Surgery Breakdown
Which Doctor to Consult for Cancer? Complete Guide to Choosing the Right Specialist
Understanding Esophageal Cancer Treatment: A Detailed Guide
Side Effects During Blood Cancer Treatment: And How to Manage Them
Second Opinion Guide: When to Consult a Medical Oncologist in India
Surgery Options in Lung Cancer Treatment in India: VATS vs Robotic vs Open
How to Compare Hospitals for Affordable Cancer Treatment in India
Head & Neck Cancer Treatment in India: Symptoms, Staging & First Steps
Stage IV Cancer: Why It's Not Always a Terminal Diagnosis
Importance of Early Diagnosis in Ewing’s Sarcoma
Who Is More Likely to Develop Salivary Gland Cancer?
Salivary Gland Cancer in Children: What Parents Need to Know
Types of Childhood Leukemia: ALL vs. AML Explained
Squamous Cell Carcinoma vs Basal Cell Carcinoma: Key Differences
Meningioma Brain Tumor: Causes, Symptoms and Treatment
Different Types of Bile Duct Cancer: Intrahepatic, Perihilar & Distal
Role of H. pylori Infection in Stomach Cancer Development
Early Warning Signs of Squamous Cell Carcinoma You Shouldn’t Ignore
Benign vs Malignant Brain Tumors – Key Differences to Know
Common Risk Factors for Developing Neuroendocrine Tumors
How Pituitary Tumors Disrupt Your Body's Hormone Balance
Why Early Detection Matters in Hepatobiliary and Pancreatic Cancers
Prolactinomas: Symptoms, Diagnosis, and Treatment Options
Plastics and Food Packaging: A Link to Cancer?
How Sunscreen Protects Against Skin Cancer: Myths vs Facts
Genito-Urinary Cancers: Types, Symptoms, and Risk Factors
What Is a Pituitary Tumor? Symptoms, Causes, and Types
Breaking the Stigma Around Prostate and Testicular Cancer
Artificial Sweeteners: Do They Raise Cancer Risk?
Cancer-Preventive Foods vs. Cancer-Promoting Foods
Processed Foods and Preservatives Linked to Cancer Risk
Difference Between Benign and Malignant Musculoskeletal Tumors
Soft Tissue Sarcoma: Types, Symptoms & Treatment
Breast Cancer During Pregnancy: Risks and Management
Importance of Self-Examination in Breast Cancer Detection
Early Signs of Bladder Cancer You Shouldn’t Ignore
How Multiple Myeloma is Diagnosed: Tests and Procedures
Early Warning Signs of Thoracic Cancers You Shouldn't Ignore
7 Pancreatic Cancer Signs You Should Know
Lung Cancer in Non-Smokers: What You Need to Know
Common Myths About Stage 4 Cancer – Debunked
Early Warning Signs of Ovarian, Cervical, and Uterine Cancers
How AI is Assisting Oncologists in Making Critical Decisions
Top 10 Tips to Minimize Harmful Compounds When Cooking in an Air Fryer
What Are Foods to Avoid While on Chemotherapy
Is a Full-Body Scan Effective at Detecting Cancer?
Top 5 Oils for Safe, Cancer-Free Cooking
Can Reusing Cooking Oil Increase Cancer Risk?
Do Air Fryers Cause Cancer?
Is Reheating Food in Plastic Containers increases Cancer Risk?
Are Induction Stoves and EMF Exposure Linked to Cancer?
12 Cancer Causing Foods You Must Avoid
Is Your Fridge Silently Raising Your Cancer Risk?
Skin Cancer Treatment in India: Key Things You Need to Know
Seeking Second Opinion From the Best Cancer Hospital in Kota
Lung Cancer Treatment in Gurgaon: Recent Developments and Treatment Options
Female Cancer Treatment in India: Why Ovarian Cancer Needs Early Detection
Choosing the Best Medical Oncology Hospital in India: Key Factors to Consider
Cancer Hospital in Raipur: A Patient Guide to Informed Choice
Importance of Regular Screening for Early Detection of Neuroendocrine Tumors
How AI is Helping Detect Rare Cancers that Often Go Unnoticed
10 Risk Factors for Colon Cancer You Need to Know
Types of Neuroendocrine Tumors and How They Differ
Gynecologic Cancer and Fertility: What Women Need to Know
Uterine Cancer: Risk Factors Every Woman Should Know
How Smoking Increases the Risk of Bladder Cancer
Myths and Facts About Lung Cancer You Should Stop Believing
Breaking the Stigma Around Stage 4 Cancer
4th Stage Cancer: What It Really Means for Patients and Families
Top Causes of Lung Cancer Beyond Smoking
Early Warning Signs of Bladder Cancer You Shouldn’t Ignore
Lifestyle Changes to Reduce Your Risk of Pancreatic Cancer
What Are Some Common Misconceptions About Lymphoma?
Early Signs of Lymphoma You Shouldn’t Ignore
Early Warning Signs of Hodgkin Lymphoma You Shouldn’t Ignore
10 Myths and Facts About Prostate Cancer
Cancer Screening for Men: Don't Ignore These Silent Threats
How AI and Technology Are Shaping the Future of Cancer Screening
Cancer Screening for Women: A Complete Guide
Acute Myeloid Leukemia in Children vs. Adults: Key Differences
Early Warning Signs of Acute Myeloid Leukemia
10 Common Myths and Facts About Leukemia
Childhood Leukemia: What Parents Should Know
Early Warning Signs of Lymphoma You Shouldn’t Ignore
Is Stomach Pain a Sign of Cancer? When to See a Doctor
Role of Palliative Care in Cancer Treatment
How Early Palliative Care Improves Quality of Life
10 Common Myths About Cancer You Should Stop Believing
Only Women Get Breast Cancer: Busting Gender Myths
12 Common Myths and Facts About GI Cancer
10 Early Signs of Pancreatic Cancer
Early Detection of Pancreatic Cancer
Early Detection of Prostate Cancer: Why It Saves Lives
How Often Should Men Get Screened for Prostate Cancer?
Is Liver Cancer Always Linked to Alcohol?
Importance of Pap Smear and HPV Tests in Preventing Cervical Cancer
12 Early Signs of Gynecologic Cancers Women Should Never Ignore
What Are Gynecological Cancers? Types, Symptoms & Risk Factors
How Often Should You Get Screened for Colorectal Cancer?
Non-Smokers Get Lung Cancer Too: Here's Why
10 Warning Signs of Colorectal Cancer You Shouldn’t Ignore
Top 5 Benefits of Early Lung Cancer Screening
Debunking Myths About Cancer Screening
Top 5 Most Common Cancer Screenings Everyone Should Know
Throat Cancer Symptoms vs Common Cold: How to Tell the Difference
Microwaves and Cancer Risk: Separating Myths from Facts
Can a Lump Behind the Ear Be Cancer? What You Should Know
Can a Hard Lump Behind the Ear Be a Tumor? Here's What You Need to Know
Brain Tumor Myths vs Facts: Can You Really Prevent Them?
Bone Cancer Symptoms vs Arthritis: How to Tell the Difference
Family History and Genetic Mutations: The Silent Risk for Young-Onset Cancer
How to Stay Active During Cancer Treatment
What to Know About Skin Cancer Screening
Who Should Be Screened for Ovarian Cancer and When?
Why Are Cancer Rates Rising Among Young Adults?
Are Processed Foods and Modern Diets Fueling Cancer in Young People?
Could Inactivity Be a Cancer Risk Factor?
Why Regular Dental Checkups Are Crucial in Detecting Oral Cancer Early
Oral Cancer Screening: Who Needs It and How It’s Done
Does Your Diet Increase Your Risk of Stomach Cancer?
Is a Full-Body Scan Effective at Detecting Cancer?
Myth vs. Fact: Common Misconceptions About Head and Neck Cancers
What is a Gastrointestinal Stromal Tumor (GIST)? Causes, Symptoms, and Diagnosis
What's the Difference Between GIST and Other Gastrointestinal Cancers?
Early Detection of GIST: What Signs Should You Not Ignore?
8 Common Side Effects Your Body May Experience During Chemotherapy
Questions to Ask Your Oncologist Before, During, and After Treatment
What Is Targeted Therapy for Cancer?
Side Effects of Radiation Therapy and How to Manage Them
What’s the Difference Between Immunotherapy and Chemotherapy?
What Is Cervical Cancer? Causes, Symptoms, and Early Detection
Bone Cancer vs. Sarcoma: What’s the Difference?
How Sarcoma is Diagnosed: Tests and Procedures Explained
Sarcoma: Types, Causes, and Symptoms
Common Myths and Facts About Sarcoma and Bone Cancer
Why Early Detection of Liver Cancer Saves Lives
Top Warning Signs of Cervical Cancer You Shouldn’t Ignore
Stages of Ovarian Cancer: What You Need to Know
Testicular Cancer in Young Men: What You Need to Know
Early Signs of Head and Neck Cancer You Should Never Ignore
How Genetics Influence Cancer Risk
What Is Palliative Care and What You Need to Know
10 Most Common Cancer Types
What are the 5 warning signs of testicular cancer?
Kidney cancer: Symptoms, treatment, and stages
Side Effects of Radiation Therapy and How to Manage Them
Bone marrow cancer: Causes, Symptoms and Treatments
Warning signs of cancer: When to see a doctor
How to Perform a Breast Self-Exam
What is the difference between targeted therapy and traditional chemotherapy?
Stages of Breast Cancer and Their Treatment Options
Oral Cancer Screening: Why Regular Check-Ups Are Crucial
Everything You Need to Know About Mammograms for Breast Cancer Screening
Foods to Lower Your Cancer Risk
Early Detection of Kidney Cancer: Why Regular Screening Matters
Understanding the Effects of Chemotherapy on Your Body
What Is Targeted Therapy for Cancer?
Common Symptoms of Colon Cancer and When to Seek Help
When Abdominal Pain Might Be More Than Just a Stomach Issue
The Importance of Choosing the Right Cancer Treatment Centre in Rajasthan
Everyday Tips to Avoid Cancer
Finding the Best Cancer Hospital in Haryana – Advanced Cancer Care, Diagnosis & Treatment
Guide to Brain Tumor Care: Top Cancer Treatment Hospital in India
How Genetics Can Influence Your Cancer Risk
How Stress and Mental Health Impact the Chances of Getting Cancer
How to Find the Right Surgical Oncologist in India for Cancer Treatment
How to Select the Best Cancer Hospital in Imphal – Important Factors to Consider
How Your Lifestyle Choices Can Increase Cancer Risk
Liver Cancer Treatment in Hyderabad: Choosing the Best Hospital
Seeking Second Opinion in Hisar for Cancer: Important Factors to Consider
Surgical Oncology Hospital in India: A Detailed Guide to Finding the Right Cancer Hospital
The Best Cancer Hospital in Vijayawada: A Comprehensive Guide
Understanding Cancer, its Causes, and Types of Treatment
How Cigarette Smoking and Alcohol Consumption Increase Cancer Risk
A Comprehensive Guide to Brain Tumor Treatment in India: Treatment Options and Innovations
Affordable Cancer Treatment in India: How to Choose the Right Cancer Hospital
All You Need to Know About Cancer Screening in Ludhiana
Best Cancer Hospital in Coimbatore: Important Factors to Consider
Best Cancer Hospital in Hyderabad: A Detailed Guide
Best Cancer Hospital in Imphal: Comprehensive Care for Cancer Patients
Best Cancer Hospital in Ludhiana: Comprehensive Care for All Types of Cancer
Best Cancer Hospital in Nagpur: Comprehensive Care for Cancer Patients
Best Cancer Hospital in Sri Ganganagar: A Comprehensive Guide
Best Cancer Hospital in Sri Ganganagar: Your Guide to Quality Cancer Care
Best Cancer Hospital in Vijayawada: An Overview to Comprehensive Cancer Care and Treatment
Best Cancer Treatment in India: Advanced and Affordable Options
Brain Tumor Treatment in Gurgaon: A Guide to Affordable Cancer Treatment
Chemotherapy: What Every Cancer Patient Should Know
Best Cancer Hospital in Punjab: Understanding Cancer Treatment Methods and Approaches
How Colon Cancer is Linked to Other Gastrointestinal Diseases
How Breast Cancer is Diagnosed: Tests, Biopsies, and More
Breastfeeding and Breast Cancer Risk: Myths vs. Facts
Early Warning Signs of Cervical Cancer You Shouldn’t Ignore
Can Diet and Lifestyle Changes Help Fight Cancer?
How Physical Activity Can Reduce Cancer Risk
Role of Nutrition in Cancer Prevention and Treatment
Top 5 Foods That Can Trigger Cancer
Role of Diet in Preventing Stomach Cancer: Foods to Include and Avoid
How to Cope with the Emotional Effects of Cancer Diagnosis
Importance of Palliative Care for Cancer Patients
Prostate Cancer: Early Signs, Diagnosis, and Treatment
Top 7 Processed Foods That Can Increase Cancer Risk
Lactate Dehydrogenase (LDH) Test: Why It Matters in Lymphoma Diagnosis
Kidney Cancer: Early Detection and Treatment Options
Skin Cancer Treatment Options: Surgery, Radiation, and Chemotherapy
How Early Detection of Prostate Cancer Saves Lives
Symptoms of Colon Cancer: When to See a Doctor
Top 10 Lifestyle Habits That Can Increase Your Cancer Risk
Are Your Cooking Oils Increasing Cancer Risk?
How Artificial Sweeteners Can Trigger Cancer: Is There a Link?
How Alcohol Increases Your Risk of Cancer: Facts You Need to Know
Ten Foods That Can Help in Prevention of Cancer
Impact of Ovarian Cancer on Fertility
Early Detection of Ovarian Cancer: Why Regular Screening Matters
Surgical Options for Breast Cancer: Lumpectomy vs. Mastectomy
Why Early Diagnosis Matters in Blood Cancer Treatment
Understanding Melanoma: Is It the Most Dangerous Type of Skin Cancer?
Understanding HPV: The Leading Cause of Cervical Cancer
Top Cancer-Fighting Foods to Include in Your Diet
The Future of AI in Oncology: What’s Next?
The Best Anti-Cancer Spices to Include in Your Diet
Skin Cancer Myths vs. Facts: What You Should Know About Treatment
Second-hand Smoke and Cancer: The Hidden Danger to Non-Smokers
Multiple Myeloma: Causes, Symptoms, and Advances in Treatment
How AI is Revolutionizing Early Cancer Detection
How Brain Tumors Affect Cognitive Function and Memory
How Lifestyle Changes Can Reduce the Risk of Breast Cancer
How to Identify Breast Cancer in Women and Men
How to Reduce Your Risk of Developing Mouth Cancer
Malignant Tumors: Causes, Symptoms, and Treatment Options
Mouth Cancer vs Common Oral Issues: How to Spot the Difference
Non-Melanoma Skin Cancer: Is It Always Curable?
Immunotherapy: The Future of Cancer Treatment?
Debunking Common Myths About Breast Cancer
Cervical Cancer Screening: Why Pap Smears and HPV Tests Matter
Can Stage 4 Cancer Be Cured?
Breast Cancer in Young Women: Unique Challenges and Risks
Alcohol and Cancer Prevention: How Much Is Too Much?
World Cancer Day 2025: A Global Call to Action
Sexual Health and Ovarian Cancer: Exploring the Connection
Signs You Shouldn't Ignore: Early Symptoms of Oesophageal Cancer
The Risks of Occasional Smoking: Can It Lead to Lung Cancer?
The Role of STIs in Ovarian Cancer Risk and Prevention
What is Nephrectomy? A Guide to Kidney Cancer Surgery
Radiation Exposure from Mobile Phones: Separating Facts from Myths
Managing One Kidney After Nephrectomy: Lifestyle Adjustments
The Link Between Junk Food and Colorectal Cancer: What You Need to Know
Occasional Drinking: Is It Harmless or a Step Towards Liver Cancer?
Breaking Down Myths: Occasional Smoking vs. Regular Smoking and Cancer Risks
Processed vs. Fresh: How Food Choices Impact Colon Cancer Risk
Esophageal Cancer: Symptoms, Causes, and Diagnosis
Partial vs. Radical Nephrectomy: Which is Right for You?
Impact of Esophageal Cancer on Swallowing and Nutrition
HPV and Ovarian Cancer: What Women Need to Know
How Smoking and Alcohol Increase the Risk of Esophageal Cancer
How Safe Are Mobile Phones When Kept Near You While Sleeping?
EMF Radiation and Cancer Risks: What You Need to Know About Mobile Usage
Signs You Shouldn’t Ignore: Early Detection of Kidney Cancer
Does Sexual Activity Increase the Risk of Gynecologic Cancers?
Does Eating Junk Food Regularly Put You at Risk for Colorectal Cancer?
Can Kidney Cancer Be Prevented? Myths and Facts
Alcohol and Liver Cancer: Understanding the Connection
Can Acid Reflux Lead to Oesophageal Cancer? Understanding the Connection
How to Differentiate Between Breast Infections and Cancer-Related Redness
Redness on the Breast: Could It Be an Infection or Cancer?
Can Irritation Be an Early Sign of Breast Cancer? Myths vs. Facts
Understanding Tests for Nipple Discharge and Breast Cancer Detection
Role of Inflammation in Breast Irritation and Breast Cancer
How to Differentiate Between Normal Testicular Changes and Cancer
Link Between Nipple Discharge and Breast Cancer: Signs to Watch For
Inflammatory Breast Cancer: Symptoms and Early Warning Signs
The Hidden Health Risks of Excessive Alcohol Consumption
Breast Shape Changes: What’s Normal and What’s Not
Breast Shape and Cancer Risk: Separating Myth from Reality
How to Differentiate Between Lung Cancer and Other Respiratory Issues
What Does Blood in the Cough Indicate? Causes and Concerns
Understanding the Role of Surgery, Radiation, and Chemotherapy in Bone Tumor Care
Understanding Bone Tumors: Types, Causes, and Treatments
Risk Factors for Uterine Cancer: Are You at Risk?
Lung Cancer and Hemoptysis: Early Signs and Symptoms
How Much Alcohol Is Too Much? Understanding Safe Limits
Headaches and Vomiting: Brain Tumors or Something Else?
Common Symptoms of Testicular Cancer and Their Causes
Early Detection of Testicular Cancer: Tests and Screenings
Early Signs of Brain Tumors: Recognizing Persistent Symptoms
When Persistent Headaches Could Be a Sign of a Brain Tumor
What Happens During a Lung Cancer Screening? A Step-by-Step Guide
Alcohol and Cancer Risk: What You Need to Know
Understanding Genetic Factors in Lung Cancer: Can It Run in Families?
The Role of Genetics in Bone and Soft Tissue Sarcomas: Are You at Risk?
The Power of Preventive Screenings: Are You at Risk for Lung Cancer?
Sarcomas in Unexpected Places: How Soft Tissue Sarcomas Develop in the Body
Myths vs. Facts: Can Birth Control or Pregnancy Lower the Risk of Ovarian Cancer?
Myths and Realities: Does a High-Fiber Diet Fully Prevent Colorectal Cancer?
Myth vs. Fact: Does Only Smoking Cause Lung Cancer?
Lung Cancer in Non-Smokers: Exploring Environmental and Genetic Causes
Understanding the Role of Gut Health: Can Probiotics Reduce Colorectal Cancer Risk?
Understanding the Silent Symptoms: How to Spot Ovarian Cancer Early
What Makes a Good Donor Match? Understanding Compatibility Beyond Family
Why Ovarian Cancer is Hard to Detect Early: Medical Insights and Myths
Is Family History Always a Factor? Understanding Hereditary vs. Sporadic Ovarian Cancer
Is Bone Marrow Donation as Painful as It Sounds? Debunking Myths Around the Process
Hidden Symptoms of Soft Tissue Sarcomas: Signs That Often Go Unnoticed
Genetic Testing for Ovarian Cancer: Who Should Get Tested and Why?
Genetic Testing for Colorectal Cancer: Who Should Get Tested?
A Parent’s Guide to Pediatric Bone Marrow Transplants: Myths, Facts, and Emotional Support
Myth-Busting: Are E-Cigarettes Safer Than Traditional Cigarettes?
Beyond the Colon: Understanding How Colorectal Cancer Can Spread
Bone Marrow Transplant Myths: Does a Match Have to Come from Family?
Bone Marrow vs. Stem Cell Transplants: What’s the Difference and Why It Matters
Bone Sarcomas vs. Soft Tissue Sarcomas: What’s the Real Difference?
Debunking Myths About Bone and Soft Tissue Sarcomas: What’s Fact and What’s Fiction?
Bone Marrow Transplants for Non-Cancerous Conditions: What You Need to Know
Pelvic Cancer and Fertility: What Women Should Know Before Treatment
Lung Cancer: Overview, Symptoms & Causes, Diagnosis & Tests, Prevention
Inflammatory Breast Cancer vs. Mastitis: How to Differentiate Between the Two
How Radiography Helps Detect Cancer: The Power of Imaging
How Diet and Lifestyle Influence Renal and Urinary Cancer Risk
How Air Pollution Contributes to Lung Cancer: What You Need to Know
From Diagnosis to Treatment: The Role of Nuclear Medicine in Neuroendocrine Tumors
Early Signs of Renal Cancer: What You Need to Know About Silent Symptoms
Does stomach cancer cause hair loss?
Chronic Kidney Disease and Renal Cancer: Understanding the Link
Breast cancer symptoms one must never ignore
Are all cysts considered tumors?
Is stomach cancer curable in stage 2?
Radiography in Radiation Therapy: A Behind-the-Scenes Look at How It Works
The Role of Radiation and Chemotherapy in Treating Tonsil Cancer
Understanding the Role of Immunotherapy in Renal and Urinary Cancers
Understanding Pelvic Cancer A Look at Cancers That Originate in the Pelvic Region
Understanding Neuroendocrine Tumors: Why Early Diagnosis is Crucial
Tonsil Cancer in Non-Smokers: What’s Fuelling the Increase in Cases?
Tonsil Cancer and HPV: Understanding the Connection
Tips to prevent Colorectal Cancer
The Role of Targeted Therapy in Treating Inflammatory Breast Cancer
The Connection Between Diabetes and Pancreatic Cancer: What You Need to Know
Symptoms of Tonsil Cancer: What to Watch for Beyond a Sore Throat
The Role of Diet in Stomach Cancer Prevention: What You Should Eat and Avoid
Living with Thoracic Cancer: Managing Symptoms and Improving Quality of Life
Managing Kidney Function After Renal Cancer Treatment
Side Effects of Radiation Therapy: How to Manage Them Effectively
Mental Health Support for Cancer Patients: Why Emotional Well-being Matters
Navigating the Emotional Impact of a Stomach Cancer Diagnosis
Palliative Care for Lung Cancer: How Radiation Therapy Can Provide Relief
Prostate Cancer In Younger Men What You Should Know About Diagnosis And Treatment
Prostate Cancer Recurrence: What Patients Should Know About Long-Term Monitoring
Prostate Cancer Screening: When and Why You Should Get Tested
Renal Cancer Survival Rates: How Early Detection Can Improve Outcomes
Risk Factors for Head and Neck Cancer: How Lifestyle Changes Can Reduce Risk
Role of Chemotherapy in Treating Advanced Cervical Cancer
Role of Early Detection in Improving Liver Cancer Survival Rates
Understanding the Link Between Diet and Gastrointestinal Cancer Risk
Living with a Brain Tumor: Coping Strategies for Patients and Families
Gastrointestinal Cancer: The Importance of Colonoscopies and Other Screening Tests
Head and Neck Cancer: Post-Treatment Rehabilitation and Voice Recovery
Liver Cancer Prevention: Lifestyle Changes That Make a Difference
Coping with Stomach Cancer: Nutritional Strategies for Patients Undergoing Treatment
Combining Radiation and Chemotherapy: A Powerful Approach in Oncology
Chemotherapy vs. Immunotherapy: Key Differences in Medical Oncology
Brain Tumor Symptoms: How to Recognize the Early Signs
Connection Between Chronic Stress and Liver Cancer Risk
Breast Cancer in Younger Women: What You Need to Know
Managing Anxiety and Depression in Cancer Patients: A Guide for Caregivers
Treatment Options for Bone Cancer
Triple-Negative Breast Cancer: Symptoms and Treatment
Understanding Non-Small Cell vs. Small Cell Lung Cancer
Understanding the Link Between Hepatitis and Liver Cancer
The Role of Diet and Lifestyle in Liver Cancer Prevention
The Importance of Regular Mammograms: When and Why to Get Screened
The Impact of Smoking on Lung Cancer Risk: Facts vs. Myths
Smoking and Alcohol: How They Contribute to Head and Neck Cancer Risk
The Role of Thyroid Hormone Replacement After Thyroid Cancer Surgery
The Role of Stem Cell Transplants in Treating Blood Cancer
The Role of PSA Testing in Prostate Cancer Detection
The Role of MRI and Other Imaging Techniques in Brain Tumor Diagnosis
The Role of Genetics in Ovarian Cancer: Understanding BRCA Mutations
The Importance of HPV Vaccination in Preventing Cervical Cancer
How Blood Cancer is Diagnosed: Tests and Procedures Explained
The Impact of Prostate Cancer on Sexual Health: What You Should Know
Lymphoma in Children: What Parents Need to Know
Mesothelioma and Asbestos Exposure: What You Need to Know
Genetic Testing and Family History: Pancreatic Cancer Risk Factors
Early Detection of Head and Neck Cancer: Warning Signs to Watch For
Early Detection of Cervical Cancer: Pap Smears and Beyond
Early Detection and Screening for Gynecological Cancers
Diet and Nutrition Tips for Pancreatic Cancer Patients
Understanding the Different Types of Lymphoma: Hodgkin vs. Non-Hodgkin
The Link Between Radiation Exposure and Thyroid Cancer
What's the best diet for Prostate Cancer?
What are the side effects of radiation therapy for lung cancer?
Does the treatment for Head & Neck cancer impair a patient's speech quality?
The role of genetics in Appendix Cancer
What Type of Foods Causes Colorectal Cancer?
Which Stage of Cancer Needs Chemotherapy Treatment
Why Smokers Need to Get Screened for Lung Cancer?
Squamous Cell Carcinoma
Role of imaging technologies in the treatment of cancer?
Ovarian Cancer Risk Rises with Obesity
Is Mastectomy the only option for breast cancer patients?
Is a constant cough a sign of lung cancer?
Green Tea and Cancer: How a Simple Cup Could Be Your Best Defense
Can someone have prostate cancer for years without knowing?
Chemotherapy and Hair Loss: What to expect during treatment?
Can Frequent Brushing or Not Brushing Teeth at All Lead to Oral Cancer?
Are Mammograms Safe While Breastfeeding?
Early signs of thyroid cancer
Does Breast Cancer Affect Only Postmenopausal Women?
Does Kidney Stones Cause Bladder Cancer?
Do Cellphones Cause Brain Cancer?
Effects of radiation therapy on Hair Loss
Importance of Early Detection in Appendix Cancer
Appendix Cancer: Overview, Symptoms, Diagnosis, and Treatment
Can severe shoulder pain be a sign of lung cancer?
AOI: A Comprehensive Guide to Most Affordable Cancer Treatment in India
Spotting the Differences Between Cysts and Tumors
Could Blood in Urine Be a Sign of Prostate Cancer?
Understanding Lung Cancer Genetics
Where does metastatic lung cancer spread to?
The best food to eat when you have breast cancer
The link between Insomnia and Cancer Treatment
The Role of Tobacco and Alcohol in Mouth Cancer Development
Vitamin D and Breast Cancer: Are they linked?
Penile Cancer: Overview, Symptoms & Causes, Diagnosis & Tests
Link between Smoking and Bladder Cancer
Is Leukemia and Lymphoma the same thing?
Is Colon Cancer hereditary?
How to manage possible side effects of Radiation for Prostate Cancer?
How does Liver Cancer affect the skin?
Colorectal Cancer Screenings: Endoscopy Vs Colonoscopy Vs Sigmoidoscopy
Does Cirrhosis increase the risk of developing liver cancer?
Does vaping cause lung cancer?
Genetic Testing for Ovarian Cancer: BRCA1 and BRCA2 Mutations
How long does it take Colon Cancer to grow?
Carcinoma Vs Sarcoma: What's the difference?
Can Hair Dye increase the Cancer Risk?
7 warning signs of Testicular Cancer
Cancer Fatigue: Overview, Symptoms & Causes, Diagnosis & Tests
Bone Cancer: Symptoms, Signs, Treatment, Causes & Stages
11 common early signs of Stomach Cancer
Types of Non-Cancerous Brain Tumors
Stomach Cancer: Causes, Symptoms, Diagnosis & Treatment
Testosterone and Prostate Cancer: Is There a Link?
Signs You Need to Schedule a Prostate Cancer Screening
Prostatitis Vs Prostate Cancer: What is the relation?
Pap Smear Test: A Lifesaver's Guide to Women's Cervical Health Screenings
Understanding Nuclear Medicine: Revolutionizing Cancer Diagnosis and Treatment
Multiple Myeloma vs. Leukemia: Understanding the Differences and Similarities
Understanding the Link Between Lung Cancer and Back Pain
Leukemia in Children: Symptoms, Causes, Diagnosis & Treatment
How Immunotherapy Works to Treat Cancer?
Chemotherapy Vs. Radiation Therapy: What’s the Difference?
Early Signs & Symptoms of Oral Cancer: Monitoring Your Oral Health
Is Head and Neck Cancer Hereditary?
How Obesity Increases the Risk of Liver Cancer?
Kidney Cancer: Symptoms, Signs, Causes & Treatment
Can Testicular Cancer Affect Fertility?
Brain Tumors in Children: 8 Warning Signs You Should Know
Brain Cancer: Types, Causes & Diagnosis
Are Women More Affected by Cancer than Men in India?
Vaping vs. Traditional Smoking: Long-Term Effects and Health Risks
Warning signs of colorectal cancer in young adults
What is the role of Image guided Radiation Therapy in Treating Cancer?
10 cancer symptoms men shouldn't ignore
10 Common Myths About Radiation Therapy Busted
Understanding the Difference between Psoriasis and Skin Cancer
Recurrent Breast Cancer: Causes, Symptoms, and Treatment Options
Severe Asthma & Lung Cancer: Unravelling the Connection
Understanding Cystoprostatectomy for Bladder and Prostate Cancer Treatment
Understanding Melanoma: From Causes to Treatment
Difference between a Bladder Cancer & Urinary Tract Infection
Bladder Cancer: Understanding Symptoms, Causes, and Treatment Options
Brain Tumors: Types, Risk Factors, Symptoms, and Treatment Options
Can an Anti-Inflammatory Diet Help Prevent Skin Cancer?
Can Frequent UTIs Be a Sign of Bladder Cancer?
How does Immunotherapy for Brain Cancer Work?
How Does Smoking Lead to Lung Cancer? Unravelling the Deadly Link
Importance of Early Melanoma Diagnosis
Difference Between PCOS and Ovarian Cancer
Early Signs of Mouth Cancer from Chewing Tobacco
Lung Cancer Symptoms: What You Should Know
Lung Cancer: Answers to Commonly Asked Questions
Melanoma Cancer: Debunking Myths and Revealing Facts
Multiple Myeloma: Navigating the Most Common Bone Marrow Cancer
Pediatric Brain Tumors: Causes, Symptoms, and Treatment Options
Does Smoking Cause Bladder Cancer? Unveiling the Connection
Myths & Facts about Ovarian Cancer: Unravelling the Truth
Ovarian Cancer Vs. Cervical Cancer: Symptoms, Treatments, Outlook
Ovarian Cancer: Understanding Symptoms, Diagnosis, and Treatment
Papillary Thyroid Carcinoma: Symptoms, Causes, and Treatment
Lump in Armpit: Should I Worry?
Brachytherapy: A Beacon of Hope in the Fight Against Cervical Cancer
Understanding the Link Between Cooking Oil and Cancer Risk
Understanding the Connection between Inflammation and Cancer
Understanding Testicular Cancer: Symptoms, Causes, and Treatment
Understanding Small Intestine Cancer: Types, Symptoms, and Risk Factors
Understanding Meningioma: Types, Causes, Symptoms, and Treatment
Cancer of the Cervix: A sexually transmitted infection?
Do contraceptives reduce or increase the risk of cancer?
Does Smoking Cause Colon Cancer?
Dry Shampoo and Cancer Risk
Early Signs of Stomach Cancer: Understanding the Warnings
Is it possible for oral cancer to metastasize to the brain?
Is prostate cancer inherited through family genes?
Understanding Acute Myeloid Leukemia (AML): Types, Symptoms and Risk Factors
Understanding Adrenal Cancer: Types, Symptoms, and Risk Factors
Understanding Carcinoma: Symptoms, Causes, and Treatment
Understanding Head and Neck Cancers: Not Just Another 'Lifestyle' Cancer
Understanding Lung Cancer in Women: Early Signs, Risks, and Treatment
Lump Behind the Ear: When to Be Concerned?
Understanding Oropharyngeal Cancer: Causes, Symptoms, and Risk Factors
Can Hair Relaxers and Straighteners Cause Uterine Cancer?
The Sweet Truth: Can Dark Chocolate Sweeten Your Chances Against Cancer?
Best diet for Prevention of Oral Cancer
10 Signs You Might Have Throat Cancer
Can Breast Cancer Spread to Lungs?
Is It Safe to Get Pregnant with Breast Cancer?
The Untold Truth About Cancer Transmission Through Saliva
Anal Cancer
Understanding Colon Cancer: Symptoms, Causes, and Diagnosis
How Do Endometrial Cancer and Ovarian Cancer Differ?
Unveiling the Unseen Danger: How Skin Cancer Can Be Deadly
Liver Cancer and Low Hemoglobin: Understanding the Connection
Understanding Lung Cancer Cough: Causes, Symptoms, and Treatments
The Definitive Guide to Lung Cancer Screening: Who, When, Why, and How
Lung Cancer: A Comprehensive Guide to Understanding, Detecting, and Dealing with the Diagnosis
Sun's Out, Shields Up: The Ultimate Guide to Skin Cancer Prevention
The Invisible Threat: Secondhand Smoke
The Silent Assassin of Our Skeletons: Tobacco Smoking and Bone Health
Understanding Bone Cancer – From Diagnosis to Prognosis
Understanding Skin Cancer: A Comprehensive Guide to Detection and Treatment
The Genetic Shadow on the Skin: Understanding Familial Melanoma
Understanding the Nuances: Cirrhosis vs. Liver Cancer
Understanding Cancer-Related Fatigue: Causes, Management, and Prevention
Can Breast Cancer Spread from One Person to Another? Understanding the Myths and Realities
Can a Dental X-Ray Detect Throat Cancer?
Breast Reconstruction Surgery
Demystifying Brain Tumours: Types, Symptoms, Diagnosis, and Treatment
Unveiling the Mysteries of Vulvar Cancer: Everything You Need to Know
Understanding Breast Cancer: ‘Pink’ Beyond Just a Color
Who Is Most Prone To Bone Cancer?
Understanding Lymphoma: A Detailed Look at a Cancer of the Lymphatic System
How to Diagnose and Treat Multiple Myeloma?
How to Spot Skin Cancer with the ABCDE Rule?
Is Obesity Linked to Cancer? Tips to Avoid Obesity and Reduce Cancer Risk
7 Warning Signs of Lung Cancer One Shouldn't Ignore
Meningioma: Understanding Types, Causes, Symptoms, and Treatments
Mouth Cancer: Causes, Symptoms, and Risk Factors
Understanding the: Multiple Myeloma
Understanding Pancreatic Cancer: Symptoms, Causes, Risk Factors, Diagnosis, and Treatment
Signs You Might Have Throat Cancer
The Role of Family History in Breast Cancer: Understanding the Connection
Ovarian Cancer: Early Signs, Detection & Treatment
Thyroid Cancer: An In-Depth Guide to Understanding This Silent Predator
Top 5 Tips to Prevent Colon Cancer
Understanding Chemotherapy: A Comprehensive Guide
Understanding Colon Cancer: Causes, Symptoms & Risk Factors
Are Headaches a Sign of Brain Tumors?
Are All Tumors of Kidney Cancerous?
Breast Cancer in Men: A Comprehensive Guide
Can Someone Have 2 Different Cancers Simultaneously?
Do Microwave Ovens Cause Cancer? Unveiling Facts and Busting Myths
Does Ovarian Cancer Affect Your Chances at Pregnancy?
Diagnosis and Treatment for Head & Neck Cancer
How to Cope with Hair Loss During Chemotherapy?
Understanding PET-CT scan with American Oncology Institute in Gurugram
Knowing Your Breast Cancer Lumps for Early Detection
Hereditary Breast Cancer: Genetic Factors and Risk Reduction
Gynaecological Cancers Unveiled: Types and Symptoms
Recognizing the Signs and Symptoms of Brain Cancer
Everything You Need to Know About Bile Duct Cancer Symptoms
Empowering Survivors: Life After Breast Cancer Treatment
Decoding Colorectal Cancer: Risk Factors and Early Detection
Colorectal Cancer Prevention: The Importance of Lifestyle Choices and Screenings
Colorectal Cancer in Young Adults: Risks and Early Signs
Colon Cancer: Signs & Symptoms
Breast Cancer Beyond Pink Ribbons: Myths and Facts
Brain Tumor Awareness: Types, Symptoms, and Treatment Options
Prostate Cancer in Men: Addressing Common Concerns
Navigating the Journey: Living with Lung Cancer
Understanding Thyroid Cancer: Types and Treatment Advances
Understanding Thoracic Cancer: Symptoms, Causes, and Treatment
Understanding Prostate Cancer: Early Detection and Treatment Options
Understanding Metastatic Brain Tumor – Causes, Symptoms, and Treatment
Understanding Meningioma: Symptoms, Causes, and Treatment Options
Thyroid Cancer and Pregnancy: Managing Challenges with Care
Signs and Symptoms of Small Intestine Cancer
Pelvic Cancer - Everything You Need to Know
Pelvic Cancer: A Comprehensive Guide to Diagnosis and Care
Lung Cancer and Smoking: Understanding the Connection
Understanding Liver Cancer Stages and Survival Rate
Gynaecological Cancers: Insights from American Oncology Institute, Hyderabad
Cervical Cancer: Causes, Symptoms, Prevention & Treatment
Advanced Gastrointestinal Cancer Treatments at AOI Hyderabad
Gastrointestinal Cancers: Strategies for Prevention and Treatment
Early Detection Strategies for Gastrointestinal Cancers: A Guide from American Oncology Institute, Hyderabad
Breast Cancer Care at American Oncology Institute: A Comprehensive Guide
Brain Tumours: Early Detection and Treatment by the American Oncology Institute, Hyderabad
Blood Cancers: Early Signs, Symptoms, and Detection at American Oncology Institute, Hyderabad
Blood Cancer Diagnosis and Treatment at American Oncology Institute, Hyderabad
Advancing Brain Tumour Care: American Oncology Institute Hyderabad
Understanding Rectal Cancer: Causes, Symptoms & Treatment
Understanding Pancreatic Cancer: Causes, Symptoms & Treatment
Understanding and Overcoming Breast Cancer at American Oncology Institute, Hyderabad
Understanding and Overcoming Gynaecological Cancers with American Oncology Institute, Hyderabad
Understanding Different Blood Cancers and Treatment Options at American Oncology Institute, Hyderabad
Understanding the Stages of Cervical Cancer
Vaginal Cancer: Causes, Symptoms & Treatment
Vulvar Cancer: Causes, Symptoms & Treatment
Gastrointestinal Cancers: Symptoms and Advanced Treatments at American Oncology Institute, Hyderabad
How Often Should Women Be Screened for Cervical Cancer?
8 Life-Saving Tips for Preventing Breast Cancer from American Oncology Institute, Hyderabad
5 Reasons for Colorectal Cancer Screening at American Oncology Institute, Hyderabad
7 Strategic Approaches for Early Detection of Gynaecological Cancers
Combatting Cancer with a PET CT Scan: A Comprehensive Guide
A Comprehensive Guide on How to Reduce Side Effects of Radiation Therapy
Understanding Chemotherapy Side Effects: 18 Ways Chemo Affects You
The Silent Killer: Prostate Cancer and Everything You Need to Know
Improving Immunotherapy for Advanced Prostate Cancer: A Closer Look
Radiation Therapy for Prostate Cancer: IMRT, EBRT, Brachytherapy & More
What to Expect After Radiation Treatment for Prostate Cancer?
Understanding the Different Types of Treatment for Prostate Cancer
The Side Effects of Radiation Treatment for Cancer: What You Need to Know
A Step by Step Guide to Understanding PET Scans
Unveiling the Truth: Foods that May Increase the Risk of Cancer
Immunotherapy for Cancer: Types, Benefits and Side Effects
The Truth About Non-Smokers and Lung Cancer
The Benefits of PET CT Scan for Breast Cancer Diagnosis and Treatment
The Power of PET CT Scans: What Makes Them So Effective?
Ureteral Cancer: Causes, Symptoms, Prevention and Treatment
Exploring the Different Types of Radiation Used for Cancer Treatment
Breath by Breath: Revolutionizing Lung Cancer Treatment with Immunotherapy
Essential Facts About Oral Cancer-What Everyone Must Know
Brain Tumor Prevention – A Primer on Reducing Your Risk
Comprehensive Guide to Cancer Support Services
Bladder Cancer Treatment: Comparing Surgery and Immunotherapy
Breathing Easy: Personalized Paths in Lung Cancer Treatment
Long-Term Survivorship and Follow-Up Care in Uterine Cancer Treatment
Managing Side Effects of Radiation Therapy: Tips for Patients and Caregivers
Uterine Cancer and Fertility: Exploring Your Options for Family Planning
The Promise of Artificial Intelligence in Brain Tumor Diagnosis and Treatment
Robotic-Assisted Surgery in Kidney Cancer Treatment
Emerging Biomarkers in Bladder Cancer Treatment
Uterine Cancer Targeted Therapies: Precision Medicine Approaches
The Connection Between Air Pollution and Lung Cancer
Bladder Preservation Strategies in Cancer Treatment: Balancing Efficacy and Functionality
Multimodal Approaches to Lung Cancer Treatment
Navigating Melanoma Identification: Understanding the ABCDE Method
The Second Opinion: A Key Element in Your Cancer Journey
The Nutrition and Cancer Prevention: Understanding the Role of Diet
The Importance of Staying Hydrated for Cancer Patients
The Heat is On! Embracing Summer While Battling Cancer
Who are Radiation Oncologists? A Closer Look at this Profession
A Comprehensive Guide to Understanding and Preventing Liver Cancer
Coping with Cancer-Related Anxiety and Depression
6 Ways You Can Prevent Kidney Cancer
The Role of Diet in Kidney Cancer Prevention and Management
Lifestyle Changes that can Help Prevent Cancer
Rectal Cancer Treatment
A Unique case of Hyper-IgE Syndrome
Awareness of Risk Factors is Key to Preventing Stomach Cancer
Lung Cancer Prevention – Knowing it better
Breast Cancer – Beyond the basics
Colorectal Cancer
World Brain Tumour Day 2021
Immunotherapy in Cancer
Oral, Head and Neck Cancer Awareness and Prevention Can Save lives
Surgical Management of Breast Cancer
Know More About the Cancer
Co-relation of early detection & excellent patient outcomes!
Cervical Cancer : Questions and Answers with Radiation Oncologist Dr Rajeev Shrivastava
No Tobacco Day | Do not let Tobacco destroy your health
Breast Cancer Recurrence
Giant cell tumor of bone (Osteoclastoma)
Immunotherapy in lung cancer
Understanding Cervical Cancer
Breast cancer and radiotherapy – Exploring various aspects
Radiotherapy in Head and Neck Cancer
PET/CT SCAN
NSCLC – Type lung cancer is on rise and here’s what you need to know
Common Misconceptions About Breast Cancer
Know about gynaecological cancers and their prevalence in northern parts of India
Things you need to know about thyroid cancer
Now this: personalised cancer treatment
A complete lowdown on cancer
Early Diagnosis is key to fighting Lung Cancer
Fight breast cancer with advanced treatment
World no tobacco day
A complete low down on anemia caused by iron deficiency
Dietary habits and cancer
Steps to reduce the risk of cancer
Physical activity and cancer
Cancer Facts
Most Common Cancers Affecting Women
Cancer treatment with radiation therapy

Are Artificial Sweeteners Linked to Cancer?
2026-04-28

Fact vs Fiction: What Really Causes Cancer?
2026-04-27

Does Green Tea Help Prevent Cancer?
2026-04-23

Can Immunotherapy Cure Stage 4 Cancer?
2026-04-20

How Many Doses of HPV Vaccine Do You Need?
2026-04-03

When Do Doctors Recommend a PET CT Scan?
2026-04-02

Can HPV Vaccine Prevent Cervical Cancer?
2026-04-01

Hormonal Imbalances and Cancer Risk in Men
2026-03-31

Does Microwave Food Increase Cancer Risk
2026-03-26

Can Detox Diets Prevent Cancer
2026-03-21

Does Hair Dye Increase Cancer Risk
2026-03-20

Do Artificial Sweeteners Cause Cancer
2026-03-19

Why Many Cancers Are Diagnosed Late in India
2026-03-12

What Is Minimal Residual Disease (MRD)?
2026-03-11

Cancer in Young Adults- A Growing Concern
2026-03-11

How Biopsy Tests Confirm Cancer Diagnosis
2026-03-10

How Sleep Patterns Affect Cancer Risk
2026-03-08

Unexplained Weight Loss Could It Be Cancer
2026-03-06

Cancer Screening for People with No Symptoms
2026-03-03

7 Pancreatic Cancer Signs You Should Know
2025-09-23

Common Myths About Stage 4 Cancer – Debunked
2025-09-23

Top 5 Oils for Safe, Cancer-Free Cooking
2025-09-22

Do Air Fryers Cause Cancer?
2025-09-19

12 Cancer Causing Foods You Must Avoid
2025-09-19

Breaking the Stigma Around Stage 4 Cancer
2025-09-16

Top Causes of Lung Cancer Beyond Smoking
2025-09-15

Early Signs of Lymphoma You Shouldn’t Ignore
2025-09-15

10 Myths and Facts About Prostate Cancer
2025-09-12

Cancer Screening for Women: A Complete Guide
2025-09-12

10 Common Myths and Facts About Leukemia
2025-09-11

Childhood Leukemia: What Parents Should Know
2025-09-11

Role of Palliative Care in Cancer Treatment
2025-09-10

12 Common Myths and Facts About GI Cancer
2025-09-09

10 Early Signs of Pancreatic Cancer
2025-09-09

Early Detection of Pancreatic Cancer
2025-09-09

Is Liver Cancer Always Linked to Alcohol?
2025-09-08

Non-Smokers Get Lung Cancer Too: Here's Why
2025-09-05

Debunking Myths About Cancer Screening
2025-09-05

How to Stay Active During Cancer Treatment
2025-07-22

What to Know About Skin Cancer Screening
2025-07-22

Could Inactivity Be a Cancer Risk Factor?
2025-07-22

What Is Targeted Therapy for Cancer?
2025-07-21

Sarcoma: Types, Causes, and Symptoms
2025-07-18

How Genetics Influence Cancer Risk
2025-07-01

10 Most Common Cancer Types
2025-07-01

How to Perform a Breast Self-Exam
2025-06-30

Foods to Lower Your Cancer Risk
2025-06-26

What Is Targeted Therapy for Cancer?
2025-06-26

Everyday Tips to Avoid Cancer
2025-06-16

How Genetics Can Influence Your Cancer Risk
2025-06-16

How Physical Activity Can Reduce Cancer Risk
2025-06-02

Top 5 Foods That Can Trigger Cancer
2025-06-02

Impact of Ovarian Cancer on Fertility
2025-05-28

The Future of AI in Oncology: What’s Next?
2025-04-23

Debunking Common Myths About Breast Cancer
2025-04-21

Can Stage 4 Cancer Be Cured?
2025-04-21

Does stomach cancer cause hair loss?
2024-11-21

Breast cancer symptoms one must never ignore
2024-11-21

Are all cysts considered tumors?
2024-11-21

Is stomach cancer curable in stage 2?
2024-11-21

Tips to prevent Colorectal Cancer
2024-11-21

Treatment Options for Bone Cancer
2024-09-20

What's the best diet for Prostate Cancer?
2024-08-21

The role of genetics in Appendix Cancer
2024-08-21

What Type of Foods Causes Colorectal Cancer?
2024-08-21
Squamous Cell Carcinoma
2024-08-13
Ovarian Cancer Risk Rises with Obesity
2024-08-13

Is a constant cough a sign of lung cancer?
2024-08-13

Are Mammograms Safe While Breastfeeding?
2024-08-12

Early signs of thyroid cancer
2024-08-12

Does Kidney Stones Cause Bladder Cancer?
2024-08-12

Do Cellphones Cause Brain Cancer?
2024-08-12
Effects of radiation therapy on Hair Loss
2024-08-12

Understanding Lung Cancer Genetics
2024-07-17

Where does metastatic lung cancer spread to?
2024-07-15

Link between Smoking and Bladder Cancer
2024-07-12
Is Leukemia and Lymphoma the same thing?
2024-07-12
Is Colon Cancer hereditary?
2024-07-12
How does Liver Cancer affect the skin?
2024-07-11

Does vaping cause lung cancer?
2024-07-11

How long does it take Colon Cancer to grow?
2024-07-11
Carcinoma Vs Sarcoma: What's the difference?
2024-07-10

Can Hair Dye increase the Cancer Risk?
2024-07-10
7 warning signs of Testicular Cancer
2024-07-10

11 common early signs of Stomach Cancer
2024-07-10
Types of Non-Cancerous Brain Tumors
2024-06-14

How Immunotherapy Works to Treat Cancer?
2024-06-10

Is Head and Neck Cancer Hereditary?
2024-06-10

Can Testicular Cancer Affect Fertility?
2024-06-07

Brain Cancer: Types, Causes & Diagnosis
2024-06-07

10 cancer symptoms men shouldn't ignore
2024-06-06
Importance of Early Melanoma Diagnosis
2024-05-15
Difference Between PCOS and Ovarian Cancer
2024-05-15

Lung Cancer Symptoms: What You Should Know
2024-05-14
Lump in Armpit: Should I Worry?
2024-04-25

Does Smoking Cause Colon Cancer?
2024-04-23

Dry Shampoo and Cancer Risk
2024-04-23

Lump Behind the Ear: When to Be Concerned?
2024-04-23

Best diet for Prevention of Oral Cancer
2024-04-22

10 Signs You Might Have Throat Cancer
2024-04-22

Can Breast Cancer Spread to Lungs?
2024-03-22

Anal Cancer
2024-03-21

The Invisible Threat: Secondhand Smoke
2024-03-21
Can a Dental X-Ray Detect Throat Cancer?
2024-03-21

Breast Reconstruction Surgery
2024-03-21
Who Is Most Prone To Bone Cancer?
2024-02-23

How to Diagnose and Treat Multiple Myeloma?
2024-02-20

How to Spot Skin Cancer with the ABCDE Rule?
2024-02-20

Understanding the: Multiple Myeloma
2024-02-20

Signs You Might Have Throat Cancer
2024-02-20

Top 5 Tips to Prevent Colon Cancer
2024-02-20

Are Headaches a Sign of Brain Tumors?
2024-02-19
Are All Tumors of Kidney Cancerous?
2024-02-19

Breast Cancer in Men: A Comprehensive Guide
2024-02-19

Colon Cancer: Signs & Symptoms
2024-01-19

Signs and Symptoms of Small Intestine Cancer
2024-01-19

Pelvic Cancer - Everything You Need to Know
2024-01-19

Understanding the Stages of Cervical Cancer
2023-12-27

Vaginal Cancer: Causes, Symptoms & Treatment
2023-12-27
Vulvar Cancer: Causes, Symptoms & Treatment
2023-12-27

The Truth About Non-Smokers and Lung Cancer
2023-12-14
6 Ways You Can Prevent Kidney Cancer
2023-10-10

Rectal Cancer Treatment
2023-01-24

A Unique case of Hyper-IgE Syndrome
2022-01-21

Lung Cancer Prevention – Knowing it better
2021-11-30

Breast Cancer – Beyond the basics
2021-10-30
Colorectal Cancer
2021-08-06
World Brain Tumour Day 2021
2021-06-18
Immunotherapy in Cancer
2021-05-13

Surgical Management of Breast Cancer
2021-04-14

Know More About the Cancer
2021-01-27

Breast Cancer Recurrence
2020-04-07

Giant cell tumor of bone (Osteoclastoma)
2020-04-01
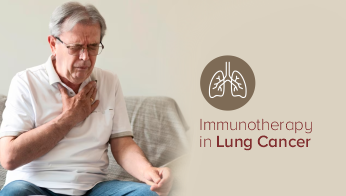
Immunotherapy in lung cancer
2020-04-01

Understanding Cervical Cancer
2020-03-13
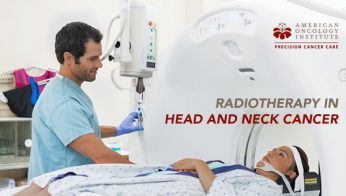
Radiotherapy in Head and Neck Cancer
2020-02-04
PET/CT SCAN
2018-11-29

Common Misconceptions About Breast Cancer
2018-10-15

Things you need to know about thyroid cancer
2018-09-12
Now this: personalised cancer treatment
2018-08-30
A complete lowdown on cancer
2018-08-16

Fight breast cancer with advanced treatment
2018-07-30

World no tobacco day
2018-05-31

Dietary habits and cancer
2018-04-05

Steps to reduce the risk of cancer
2018-04-05

Physical activity and cancer
2018-04-05

Cancer Facts
2018-04-05

Most Common Cancers Affecting Women
2018-03-28
Cancer treatment with radiation therapy
2018-03-28




